
Being treated for my Triple Negative Breast Cancer (TNBC) has felt like starting a new full-time job in this completely foreign – and toxic – industry.
The initial shock of finding the lump caused huge waves of stress and anxiety to ripple throughout my life and echo again and again in my head … much like any significant threat to your well-being … the risk of losing your job, or the fear of losing a loved one, or the trauma of wondering if your life will end. This “thing” takes over most of your headspace, leaving very little room for anything else. It’s like a shadow that creeps around in your logic, ready to overpower freedom, happiness and any other thought bubble trying to escape its darkness.
Due to Christmas and New Year holidays, vacations etc., I didn’t have my first doctor appointment-slash-interview until January 30, 2017 … almost 6 weeks after detecting something was wrong.
I was forced acknowledge it and carry its weight around with me immediately. Like considering a major career change, there were yes/no, pros/cons, I’m fine/This isn’t happening moments on the fence. You teeter one way or another … You convince yourself it’s this, then that. But you aren’t really in control … “it” is.
The first appointment was booked with my GP to get the referral to a Diagnostic Imaging clinic for Round One of testing … a mammogram and ultrasound. It was terrifying to know I had the “requirements” to go to testing. This wasn’t a lump that was easily diagnosed with no follow-up. It needed to be looked at. Stat.
Not knowing what was coming next, I continued to perform my job as a professional in the High Tech industry of computers. I was scheduled to speak to an audience in Ottawa, Ontario, Canada about Blockchain, as I was the Canadian expert. The event was planned – with me as the first speaker to kick off the session – for early February 2017. Clients, partners, and industry specialists were invited to attend. My Powerpoint presentation had approximately 40 slides to deliver in 45 minutes. I had been doing education, research, attending seminars, customer meetings, recording videos and giving presentations on the subject for over 6 months, and had become the “go to” person in Canada.
Forty-five minutes before I was boarding the train for Ottawa, I got the call that I needed to come in for a second interview ASAP … my GP wanted me to see the surgeon – Dr. X – that day!
I was focused on delivering my presentation and told my doctor that I had to go to Ottawa. There was no one who could cover for me this late in the game, and my professional training kicked in. The customer event was the following morning. So I boarded the train, went to Ottawa and checked into my hotel.
I met a colleague in the hotel lobby bistro … and could barely talk about my lump. It felt like it had moved to my throat.
“Don’t look at me that way,” I said “or I will cry.”
Both of us blinked away unshed tears on the verge of spilling. I had to look away and regain my composure. I would not let it crack now.
Alone in my room, I took less than a quarter of a sleeping pill – terrified to sleep in – and set three alarms for 6am Tuesday.
I woke up with the first alarm, felt my lump, showered and dressed. I wore a simple but classic jumper dress in pinstripe gray, smokey gray stockings and heels. I checked out of my room, went downstairs and had a simple watercress & goat cheese omelet with coffee for breakfast.

After breakfast, I headed to the hotel conference room to be mic’d up for a sound check and to run through my slides. I always like to see how they look from different distances and angles in the room to make sure everyone can see what I am talking about. For this particular presentation, I would more or less be stuck in one corner so I didn’t block the view of the screen. I usually like to move around and stand in front of different people while presenting, but didn’t trust my legs that morning. I had enough distractions without tripping over wires and power cords, so I picked a spot to the left of the screen and placed my water bottle on the podium.
Local executives, clients, and business partners were arriving, so I moved around the room for introductions and small talk. After years in this industry, I moved into a professional auto-pilot mode. I’m a trained killer. Smile. Camera. Action.
I really enjoy the work that I do and the topic I present, so i slid into my Technologista role with ease. Our executive kicked off the session, introduced me to the audience as I stepped in front of them.
Showtime! I talked for the full 45 minutes … captivating them with new concepts and interesting factoids of future technology, then bringing it home to why it matters and how our company can help them. There were questions at the end and applause as I took my leave of the front of the room.
I made an exit out the side door to sink into a chair in the main hall and decompress. Job well done, I thought. No one would believe I had just found out I had a very suspicious 7cm (sizing at the time) mass in my right breast.
I popped back into the hall to hear the other speakers, then back out to sit and decompress a little longer. Now that my speech was done, my brain could poke at the call from the doctor … maybe it was this kind of tumour … or another kind. Suspicious, but benign. I tried to think about other things.
The doors opened and the attendees filed out for the buffet lunch. I smiled, stood up and got in line to grab a plate of our catered lunch. I made my way back into the room and sat down with a table of customers so we could chat over lunch. They peppered me with questions about my topic and my views on the effects it would have. We passed out business cards and promised to get in touch later that month.
I had decided not to stay for the afternoon session, so I took my leave of the event and said goodbye. I hailed an Uber car from my phone and was at the Ottawa train station with time to spare.
Once seated in First Class, I had a coq au vin dinner with a glass of white wine (or two) and tried to read a book on my iPad. More often than not, found myself staring outside at the landscape, lost in thought. Thankfully First Class was almost empty so no one noticed my head leaning on the rain-splashed window and tears streaming down my face. The Reality Show my life had become zoomed closer and closer as the train took me home. The pretense I had kept up could now come down.
I had to come face to face with the fact … no, possibility … that the news would be bad. While I had tried to remain optimistic, it’s impossible not to think of all the outcomes. I’m a technical analyst by trade. I’m trained to dig through information and look for logical solutions. I can put two plus two together. My GP had insisted I see the surgeon immediately … that can’t be good news.
I had bouts of anxiety and stress about the callback. I would wake up at night in a cold sweat, my heart beating in fear. One moment I would be fine … the next I would be trying to find a quiet corner to ride out the panic attack. But I had to be strong. As a single Mom, I was trying to keep myself together at home and at work. The fear only seeped out the cracks when I was alone or safe with my closest friends.
The train rocked on the tracks and the sounds seemed to put me in a meditative trance, which was a good thing. I felt sad, lonely, unsure of what was coming next. I was lost in churning thoughts for hours. Checking the time on my phone, I knew we should be getting close to my stop, so I gathered up my laptop and phone. Like any true geek, I used the technology I had in my hand and fired up Waze to see where I was.

We pulled into the Oshawa Via Station to freezing rain, but I had already sent my Uber ride request so my driver was there. I was glad to be home with my son and our two dogs. The business attire came off and I slipped into a tshirt and comfy yoga pants, and poked again at that God damn lump.
The following days I had my second and third interviews … I saw my GP who somberly handed me the ultrasound report. On a scale of 0 to 5 – with 5 being highly suspect of malignancy – I was a 5. I was scheduled to see Dr. X the next morning.
When I saw Dr. X on February 9th, I asked him if he suspected this was cancer. His answer was simple and direct.
“Yes.”
I was starting to think I had the job.
I put on a brave face and continued my socialite lifestyle the very next day … Wearing a red wig for Sue’s birthday bash at the Edge. The wig was such a hit, that I wore it to another Red-and-White Pub event the following night. And again on Valentine’s Day. I was doing my best to stay positive and hopeful. Que sera, sera … whatever will be, will be.
I had one more step to confirm I was perfect for the role as a breast cancer patient. A needle biopsy was performed on the Friday after Valentine’s Day. While I was admitted to the hospital, put in an ugly blue gown and prepped for having a large needle stuck in my breast, friends were boarding a plane in their shorts and flip flops for a fun-filled Caribbean vacation. My girlfriends called and begged me to hit the clubs with them … “C’mon!” they said. “We can head downtown and dance all night!”
My breast was bleeding and badly bruised from the needle, so all I wanted was to put it on ice and take pain medication. The last thing I needed was to get elbowed in the chest on a crowded dancefloor.
Suddenly I realized that my life was about to drastically change. While everyone else got to continue on with their wonderful lives, mine was derailing right of the tracks.
It was a tough pill to swallow, and I started to slide down that old rabbit hole of depression … I sobbed uncontrollably. I threw things at the wall. I yelled at my family. I drank far too much wine. I was desperate to hang on to the past, but people, places and good times were slipping through my fingers. It was a pity party that swirled lower and lower. That will be another post …
On the tenth day after the biopsy, I arrived at Dr. X’s office for my biopsy follow-up with my long time friend Terri beside me. She held my hand and squeezed to let me know she was there.
I got the job. I had a (resized) 3.5cm tumour of highly Invasive Ductal Carcinoma.
Dr. X fit me in for surgery as soon as possible so it was scheduled for March 10 – on what would have been my Father’s 94th birthday.
Fran, Sue and my son Matt stayed at the hospital all day. While I was under general anesthetic on the operating table, they were taking selfies and sending them to my iPhone. I love these people!

The surgery was a success! I healed so fast that seven days later I was wearing a green wig and drinking green beer to celebrate St. Paddy’s Day with my circle of friends!

I saw Dr. X for a post-surgery follow-up. Triple Negative Breast Cancer – Stage 2a/Grade 3 – 3.5cm tumour – clean margins – node negative. He was referring me to the Cancer Centre to see the oncologist for the next step in my journey.
And that is when we got down to the serious business of being a cancer patient.
I was contacted by Randy* my Care Coordinator at the R.S. McLaughlin Durham Regional Cancer Centre (DRCC) with information on my two upcoming appointments with separate oncologists for radiation and chemotherapy. It would be the first of many full days at the hospitals.
My first day started at the Ajax Hospital to meet my Radiation Oncologist … the appointments were scheduled for their convenience – not mine – because Dr. IQ dropped the bomb that I was indeed getting chemo … and lots of it.
“Oh yes,” he said. “You are getting the full load. I spoke to Dr. F this morning and she is recommending a dose dense protocol. This is highly aggressive cancer.”
He advised me of the percentages (30% chance of recurrence without radiation, 5% chance with) and what to expect in radiation, but to forget that for now. I wouldn’t see him for 4-6 months until after my chemotherapy regimen was completed. Good thing I had done my research and was prepared for that news. If I had of let myself live in denial these past few months, that first meeting would have been a harsh smack of reality. I would have been a screaming 3-year-old on the floor.
Sherri – my handler for the week – and I went to PhoMono for lunch before heading to the Cancer Centre. We enjoyed a light lunch of Rare Beef Pho and green tea, while I digested the news that I was getting chemo and radiation.
At the DRCC, my heart sank as soon as we walked in. Shit got real. These coworkers/patients were SICK! They had no hair, no smiles, no sparkle of light left in their eyes. Would that be me in a matter of weeks? Could I remain my boisterous self with red and green hair and stand out among the ashen gray of the cancerous?
I was given an identification badge so I could scan myself in each time I arrived for appointments, then sent for bloodwork.
I have an employee/patient identification # which I need to use if I call anyone on my cancer care team.
I got poked with another needle for blood … and found the condom cookie jar!

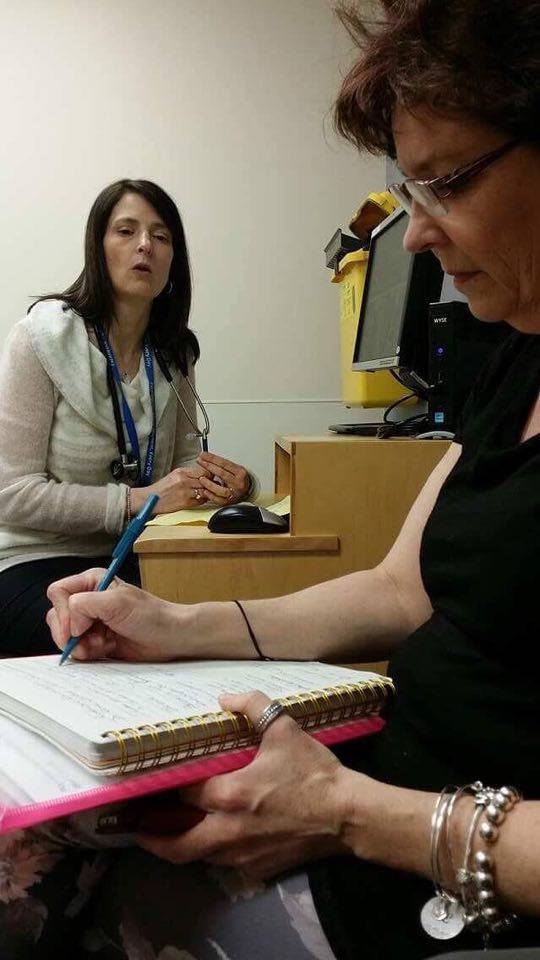
We were taken into a room where I met my Primary Care Nurse – Kaye* – who asked me if I knew where I was and why I was there … Yes! I applied for the job as a cancer patient and was awarded the prestigious position in the Triple Negative Breast Cancer department! Apparently, people arrive not knowing they already had this job or why they were here …
Kaye gave me a blue bag with a very important blue file folder which I must have with me at all times … The blue folder contained printouts of my calendar of treatments complete with instructions on how to prep for each appointment and where it was located. If I wanted to see the high tech version, I could access the online Patient Portal. New/changed appointments would be recorded my personal calendar and I could complete online follow-up surveys of symptoms. I was also given several prescriptions but told not to fill them until I had talked to a Pharmacy Coordinator. One injection for Neulasta, which boosts a natural protein to signal my body to grow new white blood cells, will cost $3000 per injection … and I needed 8 so we had to ensure I had coverage with my health plan. The other drug is called Emend, and is an anti-nausea and vomiting medication. I was hoping the steroids would be in pill form so I could not take them … but no such luck! (I refuse to gain weight … denial, denial, denial).
In addition to my identification badge, I also got a discounted parking pass for frequent flyers, and a “Go Directly to Emerg and Do Not Pass Go” Fever Card. If I show up at an Emergency Room with a fever and this card, I move the front of the line for triage (after other life-threatening emergencies, of course) and the card tells the emergency room doctor what procedures to follow.
I have a full deck of business cards for my health care team and a basic red bracelet to identify my drug allergies.
Dr. F is my oncologist. She is a top-notch doctor … Chief of Oncology and she was recently appointed to a provincial seat for systemic treatments. Dr. F and I settled into a no-nonsense discussion of protocols, statistics, and genetic testing. She is hitting my cancer with dose dense AC-T. I will get 4 infusions of the AC combo (Adriamycin and Cyclophosphamide) over the first 8 weeks, then 4 doses of T (Taxol) over the last 8 weeks … total of 16 weeks. Heavy stuff.
Did you know that 40% of cancer patients previously had cancer? And they don’t necessarily get a repeat of their original cancer. The treatment itself causes cancer … This is fucking nightmare that won’t go away.
Triple Negative Breast Cancer is a rarer, but more aggressive form, affecting only 15-20% of breast cancer patients. It’s always Invasive Ductal Carcinoma, but has no hormone or gene expression and therefore no therapies outside of chemo and radiation (ER-/PR- and HER2-). I will do genetic testing to find out if I carry the BRCA1/BRCA2 gene mutation, but there is only a 5% chance that I do.
If I do … I am at risk for new cancers in both breasts and my ovaries.
Cancer is staged by the tumour size and how far it has metastasized or moved to other sites in my body outside its point of origin. I am staged as 2a meaning my tumour is >2cm but less than 5cm – and more importantly – not in my lymph nodes.
Cancer is graded on its aggressiveness as 1 (slow growing) 2 (faster) or 3 (aggressive) … and I got the Grade 3 aggressive cancer. I have a higher chance of recurrence or death. If I chose not to do chemo, I would have a 40% risk of death in two years vs 20% if I do. At the 5-year cancer free mark, my odds simmer down to that of other breast cancer patients, which is pretty good.
I had a slew of tests set up to prove I was ready to start my job; a CT Scan, a MUGA Heart test, and a Bone test.

The CT Scan was pretty interesting – except for the part where I got sick after I drank the barium liquid … and still had to sit there for an hour waiting for it to do whatever it had to do. Once positioned on the CT Scan machine, the technician told me the dye injection would make me hot and tingly, give me a metallic taste in my mouth and the sensation of peeing my pants … but I wouldn’t really. Or I might not feel a thing. The technician put me through two dry runs in the CT Scan machine (A computer generated voice telling me to “Breathe in … Hold … Take a breath”) then let me know she was injecting the dye.
I didn’t get hot, but I got tingly.
I didn’t taste anything metallic but did feel the tingly sensation as the dye raced through the veins behind my throat … and then all the way down to my butt and between my legs. I am sure my eyes popped wide open at that sensation! It’s hard to describe and not at all unpleasant … Breathe in … Hold … Clench … Take a breath! Can we do that again?!
The CT Scan machine is like a donut that spins while it moves up along your body … I could see flashing lights and I was reminded of 2001 Space Odessey “My God! It’s full of stars!”
The next day was similar to a new employee orientation … A Welcome & What to Expect presentation and a tour. Sherri and I arrived for the 2-hour Chemo Class – listened to an 80-slide power point presentation – and went on a tour of the cancer centre.
Seeing the Systemic Unit where they deliver the chemotherapy was … terrifying. Old, young, sick, vomiting, comatose, sad, crying. The girl directly in front of me still had a head full of beautiful red hair. She was sick – vomiting and wiping her mouth – while looking up at me, as if ashamed. I looked away … to give her the privacy she needed.
I couldn’t help but think that one day soon I will be sitting in that chair looking like death warmed over and the “new recruits” will be brought in for their tour. It’s humbling, it lacks dignity and it’s horrific to witness.
I have a new respect for the person by my side because none of this is pretty to watch. Thank you to my friends who will be by my side every step of the way. I couldn’t do this without you.
We left the chemo chamber of horrors early to get to my next test … the MUGA Heart scan. But I had to make a pit stop in the nearest washroom to vomit…
The MUGA (multigated acquisition) scan measures how well my heart beats. The chemo cocktail will be incredibly hard on my heart, and I can only have so many treatments over my lifetime.

After two injections of a radioactive tracer, I am placed in another machine and told to lie still for about 15 minutes while the cameras move around ~270 degrees to take photos of my beating heart. No talking and moving allowed!

I relaxed and went to the “place” I go to when I want to talk to God. We had a pretty good conversation during those 15 minutes in the machine. The technician repositioned me – in what Sherri called bondage straps – and told me the test was taking longer because I had a slow heart beat.
“Oh!” I exclaimed. “I slowed it right down! I can speed it up if you want!”
“No … No … just let it … beat … normally.”
So God and I had another 5-minute conversation before I started to drift in and out of sleep.
Heart rate between 50 – 60 bpm … I still have the heart of an athlete!
Today I see my GP to refill my medications and Friday I am back at the DRCC for a 3-hour Bone Scan. A bone scan is a nuclear medicine imaging test that uses bone-seeking radioactive tracers – I must be glowing after all the radioactive shit that has been injected into me this week – and a computer to create an image of my skeleton. A bone scan looks at the bones to see if there are any abnormalities, such as a fracture, infection or if cancer has spread to my bones.
Fear of the unknown creeps in again … Will this fear of cancer jumping out of the shadows ever go away???
Maybe I should do my homework. I have lots and lots of reading homework. I have come home from various appointments with the following manuals to read:
Helpful Hints for the Newly Diagnosed
Breast Cancer – Understanding your Diagnosis
Exercises After Breast Surgery (cording)
Understanding Treatment for Breast Cancer
Eating Well When You Have Cancer
Chemotherapy and Other Drug Therapies
Living with Cancer
Sexuality and Cancer
Your Guide to the R.S. McLaughlin Durham Regional Cancer Centre
Safety Training
Day of Surgery, Stop the Clot!, Infection Control
Extra-curricular education:
Videos on chemo bags (what to bring with you), wig selection and care and makeup
Food for Thought Nutrition Class
Take a Breath Workshop for Stress & Anxiety
Yoga & Zumba & Tai Chi
Reiki, Massage, Reflexology
Before & After Breast Cancer
Sex Ed!
And I have to find time for an off-site meeting at the Hearth Place Cancer Centre!
Next Monday, April 10, I start my new job. I see the Pharmacy Coordinator to review the various concoctions of drugs that will be used to treat my breast cancer and make selections where I can. After that meeting, I have Pre-Tx (treatment) bloodwork and a Pre-Tx consult with my oncologist.
Tuesday, April 11 I get my PICC line inserted so they can hook me up via IV to the chemo cocktail. The PICC line is a long catheter tube that is inserted into a vein in my arm then pushed intravenously into the large vein that carries blood into my heart.
Right after that is inserted, I get my first chemotherapy infusion. I have no idea what to expect.
Wish me luck!
Cancer girl,
The Fox
*Names changed to protect the innocent!
© 2017

You impressed me when you read your own bedtime stories at 4 years old; while I scavenged for cigarette butts in your parents’ ashtrays–fyi, it took everything I had to finally break that smoking habit at 21.
But now, you simply blow me away! I’m reading YOUR story and I can’t ‘put it down’. I hope, with all my heart, that the conflict part of it resolves to a very satisfying climax 🙂 — You have this, Lisa!
LikeLiked by 1 person